Public health professionals operate within a layered system that connects neighborhoods to national institutions. Their work extends far beyond clinics and hospitals. Community educators guide families toward healthier choices. Epidemiologists analyze disease trends to detect early warning signs. Policy experts shape regulations that reduce risk across entire populations.
Emergency planners prepare coordinated responses before crises strike. Each level strengthens the next, creating a network focused on prevention first and protection when needed. Understanding how these roles connect reveals why public health remains essential to social stability and long-term well-being.
Community-Level Prevention Strategies
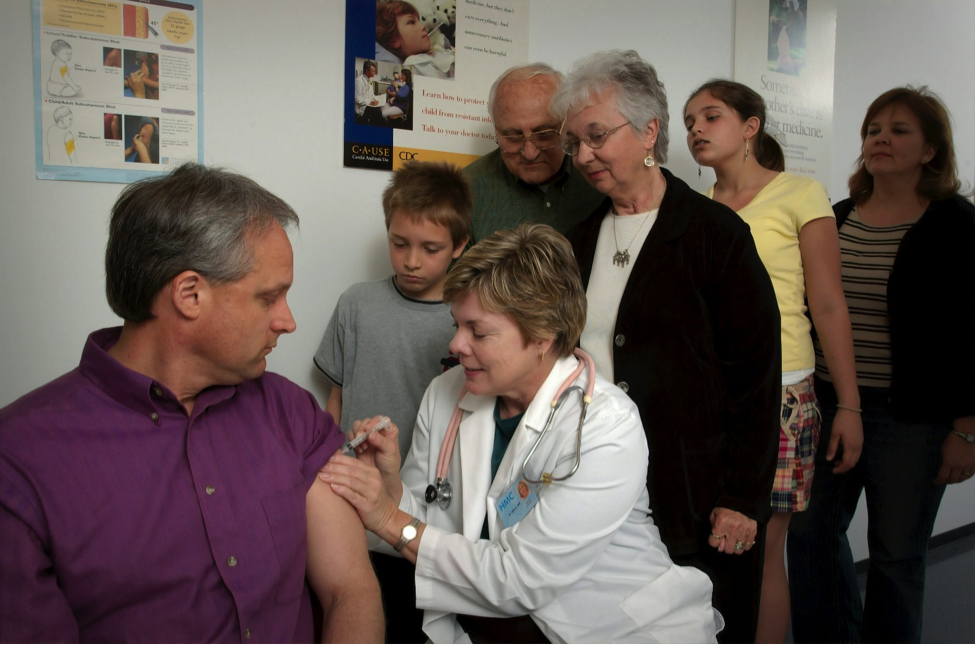
Communities serve as the front line of public health. Local departments and nonprofit organizations focus on practical interventions that address everyday health concerns. Vaccination drives, nutrition workshops, smoking cessation programs, and maternal health services all begin with an assessment of local needs. Professionals gather input from residents and community leaders to understand barriers that affect participation.
Cultural awareness shapes how messages are delivered. Outreach campaigns reflect the language, values, and traditions of the populations they serve. Trust builds gradually through consistent presence and open communication. Residents respond more positively when information comes from familiar, credible sources.
Education, Training, and Workforce Development
Effective public health systems depend on skilled professionals who understand both science and community dynamics. Academic preparation introduces future practitioners to epidemiology, environmental health, health policy, and research methods. Classroom instruction establishes theoretical knowledge that guides evidence-based decision-making.
Practical experience strengthens that foundation. Field placements expose students to real-world challenges, including outbreak investigations and community assessments. Mentorship helps early-career professionals refine judgment and leadership skills. Continuous learning remains essential because health threats evolve. A strong public health workforce has the right qualifications, comprehensive training, and ongoing professional development to address complex and evolving health challenges effectively. Investment in training programs ensures that professionals remain prepared for new diseases, technological advancements, and demographic shifts.
Data Collection and Disease Surveillance
Reliable information drives effective public health action. Surveillance systems track infectious diseases, chronic conditions, and environmental exposures. Laboratories confirm diagnoses, while digital reporting systems compile data in real time. Analysts review trends to identify unusual patterns that may signal emerging threats.
Data does more than document illness. It guides resource allocation and shapes targeted interventions. Rising asthma rates in a particular region may prompt air quality investigations. Increased rates of obesity can lead to expanded nutrition initiatives. Careful interpretation prevents overreaction while ensuring a timely response.
Policy Development and Advocacy
Research findings gain lasting impact when translated into policy. Public health professionals collaborate with legislators, educators, and industry leaders to promote standards that protect communities. Evidence supports regulations on food safety, water quality, tobacco control, and workplace protections.
Policy work requires negotiation and strategic communication. Professionals present data in ways that resonate with diverse stakeholders. They highlight long-term benefits of prevention, including reduced healthcare costs and stronger economic productivity. Community advocates often amplify these efforts by sharing lived experiences that illustrate the human impact of policy decisions.
Emergency Preparedness and Response
Public health planning anticipates potential crises before they unfold. Preparedness teams develop response frameworks for disease outbreaks, natural disasters, and other large-scale emergencies. Plans outline communication channels, supply distribution systems, and coordination protocols with hospitals and emergency services.
Training exercises simulate real events to test readiness. These drills reveal gaps in logistics or communication that can be corrected before a true emergency occurs. Rapid response depends on established relationships among agencies and clear chains of command. Crises demand both speed and accuracy. Professionals monitor evolving data, issue timely guidance, and adapt strategies as conditions change. Community trust, built through ongoing prevention efforts, becomes critical during emergencies.
Health Equity and Community Partnerships
Health outcomes often reflect deeper social and economic conditions. Income, housing stability, education, and access to transportation influence whether individuals can maintain good health. Public health professionals examine these broader factors to reduce disparities across populations. Careful analysis identifies which communities face higher risks and why those gaps persist.
Partnerships strengthen these efforts. Local schools, faith-based organizations, advocacy groups, and small businesses help extend the reach of health initiatives. Collaboration ensures that programs reflect real community priorities rather than outside assumptions. Listening sessions and advisory boards provide space for residents to share concerns and suggest solutions.
Environmental and Occupational Health Protection
Daily environments shape long-term health outcomes. Environmental health specialists monitor air quality, drinking water safety, and waste disposal systems to reduce exposure to harmful substances. Routine inspections of restaurants, public facilities, and industrial sites maintain consistent safety standards.
Workplace conditions receive similar attention. Occupational health professionals evaluate risks related to machinery, chemical exposure, and repetitive strain. Clear regulations and safety training programs reduce injuries and long-term illness among workers. Employers benefit from safer conditions through improved productivity and lower healthcare costs.
Global Collaboration and National Security
Public health challenges rarely remain confined within borders. Infectious diseases spread quickly through travel and trade. International cooperation strengthens early detection and rapid containment of emerging threats. Information-sharing agreements allow countries to report outbreaks and coordinate responses efficiently.
Global partnerships also support research and vaccine development. Collaborative studies expand scientific knowledge and improve preparedness worldwide. Strong relationships between nations contribute to collective security, since uncontrolled outbreaks in one region can affect many others. National health security depends on these global connections. Surveillance systems, laboratory networks, and coordinated response strategies create a protective framework.
Public health professionals operate across interconnected levels that move from prevention to protection. Community-based programs address immediate needs and build trust. Education and workforce development ensure that skilled practitioners guide these efforts. Data systems provide insight that shapes informed decisions. Policy initiatives create safer environments, while preparedness planning safeguards communities during crises.
Equity-driven partnerships and environmental oversight further strengthen the system. Global collaboration adds another layer of protection in a world where health risks cross borders with ease. Together, these efforts form a coordinated structure designed to reduce risk, respond effectively, and promote long-term well-being. Strong public health systems support healthier populations and more resilient societies.