According to the American College of Prosthodontists, over 3 million Americans currently have dental implants—a number growing by 500,000 annually. Yet despite their widespread adoption, persistent myths about implant longevity continue to influence patient decisions and treatment outcomes. Many people still believe implants either last forever without maintenance or fail within a few years, creating unrealistic expectations that can derail otherwise successful treatments.
These misconceptions matter more than ever in 2024, as implant technology has evolved significantly while treatment costs remain substantial. Patients investing $3,000-$5,000 per implant deserve accurate information about what truly affects long-term success. For those considering replacement options, understanding the benefits of dental implants for missing teeth can help ensure a durable, functional, and aesthetically pleasing result. The stakes are particularly high because long term dental implants represent a lifetime commitment to oral health maintenance—one that succeeds or fails based largely on understanding what makes them durable.
The reality about implant longevity sits between the extremes of “forever” and “temporary fix.” Modern implants demonstrate impressive survival rates when properly selected, placed, and maintained, but their success depends on factors many patients never hear about during initial consultations. Here’s what the research actually shows about making implants last decades, not just years.
What Are Long Term Dental Implants?
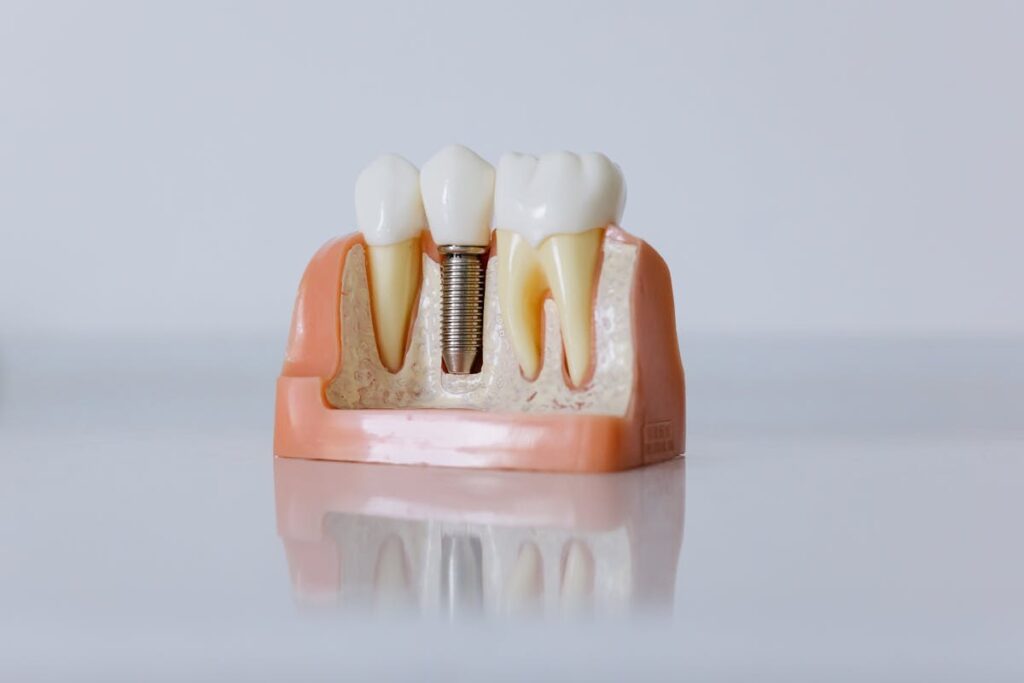
Long term dental implants aren’t a separate category from regular dental implants—they’re the same titanium or zirconia posts designed for permanent tooth replacement. The “long term” designation reflects both the intended lifespan and the treatment approach required to achieve it. Unlike temporary solutions such as removable partial dentures or short-term bridges, these implants integrate directly with jawbone tissue through a biological process called osseointegration.
This integration process distinguishes implants from every other tooth replacement option. While dentures sit on gums and bridges attach to adjacent teeth, implants become part of your skeletal structure. The titanium post functions as an artificial tooth root, supporting crowns, bridges, or dentures with stability that closely mimics natural teeth.
Current research defines implant success over decades rather than years. A 2023 systematic review in the *Journal of Dental Research* found that properly maintained implants show 95-98% survival rates at 10 years, with many functioning effectively for 20-30 years or longer. However, this longevity isn’t automatic—it emerges from careful patient selection, precise surgical placement, appropriate prosthetic design, and consistent long-term maintenance.
The distinction between successful long-term implants and failed ones often comes down to understanding what “success” actually means. Dental professionals measure success not just by whether the implant stays in place, but by bone levels around the implant, absence of infection, and functional performance over time. These criteria help explain why some patients enjoy decades of trouble-free use while others experience complications within years.
How Do Long Term Dental Implants Achieve Longevity?
Bone Integration and Healing Process
The foundation of implant longevity lies in osseointegration—the direct structural connection between living bone and the implant surface. This isn’t simply bone growing around the implant like a fence post; it’s active bone cells forming intimate contact with the implant material, creating a biological bond that can actually strengthen over time.
During the initial 3-6 months after placement, specialized bone cells called osteoblasts deposit new bone matrix directly onto the implant surface. Modern implant surfaces are deliberately roughened at the microscopic level to encourage this cellular attachment. The healing process follows predictable stages: initial clot formation, soft tissue healing, bone remodeling, and finally mature osseointegration where the implant becomes mechanically locked in place.
Research from the *International Journal of Oral & Maxillofacial Implants* demonstrates that successful osseointegration creates a bond stronger than many natural tooth-root attachments. This explains why properly integrated implants can withstand normal chewing forces for decades. However, the process requires adequate bone quality, proper blood supply, and absence of infection—factors that vary significantly between patients.
Implant Design and Material Influence
The physical characteristics of the implant itself dramatically affect long-term success. Surface technology has evolved from smooth titanium to complex micro-textured surfaces that promote faster, stronger bone integration. Current generation implants feature surfaces treated with acids, sandblasting, or specialized coatings that increase surface area and encourage cellular attachment.
Titanium remains the gold standard due to its biocompatibility and mechanical properties, but zirconia implants are gaining recognition for specific applications. A 2024 comparative study found titanium implants show slightly higher long-term success rates in posterior regions under heavy chewing loads, while zirconia performs excellently in anterior areas where esthetics matter most.
Thread design, implant diameter, and length also influence longevity. Wider implants distribute forces more effectively, reducing stress on surrounding bone. However, anatomical limitations often constrain these choices, making proper case selection crucial. The implant-abutment connection—how the crown attaches to the implant—has evolved toward designs that minimize bacterial infiltration and mechanical loosening over time.
Types and Materials Used in Long Term Dental Implants
Modern implant materials fall into two primary categories, each offering distinct advantages for long-term function. Titanium implants represent the established standard, with over 50 years of clinical documentation and survival rates exceeding 95% at 15 years. Titanium’s unique property of osseointegration was discovered somewhat accidentally in the 1960s, but decades of research have optimized its surface characteristics for maximum biological compatibility.
Zirconia implants offer an alternative that appeals to patients preferring metal-free restorations. This ceramic material demonstrates excellent biocompatibility and superior esthetics, particularly in the anterior region where gum recession might expose implant margins. However, zirconia’s brittleness compared to titanium requires careful case selection and surgical technique.
Surface treatments have revolutionized both materials’ performance. Sandblasted, large-grit, acid-etched (SLA) surfaces create optimal conditions for bone attachment by providing microscopic roughness that cells can grip. Newer surface modifications include calcium phosphate coatings and growth factor applications that theoretically accelerate integration, though long-term data remains limited compared to established surface treatments.
The choice between materials increasingly depends on specific clinical situations rather than universal superiority. Patients with thin gum tissue in visible areas often benefit from zirconia’s tooth-colored appearance, while those requiring maximum strength in posterior regions typically receive titanium implants. Understanding these material differences helps explain why implant longevity varies between patients even with identical maintenance routines.
Long Term Dental Implants Versus Bridges and Dentures
When comparing longevity between replacement options, long term dental implants consistently outperform traditional alternatives in both lifespan and functional preservation. Fixed bridges typically require replacement every 10-15 years due to failure of supporting teeth, cement failure, or secondary decay. Since bridges rely on adjacent teeth for support, they subject healthy teeth to additional stress while creating areas difficult to clean effectively.
Removable dentures face even greater longevity challenges. Complete dentures require relines every few years and full replacement every 5-8 years as jaw ridges shrink from lack of stimulation. Partial dentures place mechanical stress on supporting teeth through clasps and rests, often leading to tooth loss that necessitates denture redesign. The functional limitations of dentures—reduced chewing efficiency, speaking difficulties, and social concerns—compound over time as bone loss progresses.
Implants break this cycle of replacement and bone loss by providing stimulation that maintains jawbone density. Research from the *Clinical Oral Implants Research* journal shows that areas with implants maintain 90-95% of original bone volume over 20 years, compared to 40-60% retention in denture-wearing areas. This bone preservation advantage compounds over decades, making implants increasingly superior as patients age.
From a quality of life perspective, long-term studies consistently favor implants. Patients report greater satisfaction with chewing ability, speech clarity, and social confidence. A 2023 longitudinal study following patients for 15 years found implant recipients maintained better nutritional status and reported higher oral health-related quality of life compared to bridge or denture wearers. These functional advantages often improve rather than decline over time, contrasting sharply with the deteriorating function typical of other replacement options.
Common Myths About the Longevity of Dental Implants
Myth: Dental implants last a lifetime without any maintenance. This dangerous misconception leads to more implant failures than any other factor. While implants don’t develop cavities like natural teeth, they’re susceptible to peri-implantitis—an inflammatory condition affecting the tissues surrounding implants. Without proper oral hygiene and professional maintenance, bacterial biofilms accumulate around implant crowns just as they do around natural teeth.
Clinical evidence shows that patients who skip regular professional cleanings experience peri-implantitis rates 3-4 times higher than those following recommended maintenance protocols. The condition progresses more rapidly around implants than natural teeth because implants lack the biological defense mechanisms that natural tooth roots provide. Once established, peri-implantitis can cause rapid bone loss that threatens implant survival.
Myth: Smoking doesn’t significantly affect implant longevity. Research consistently demonstrates that smoking represents the single greatest controllable risk factor for implant failure. Nicotine restricts blood flow essential for healing and ongoing tissue health, while combustion products impair immune response around implants. A comprehensive meta-analysis published in 2024 found smokers experience implant failure rates 2.5-3 times higher than non-smokers, with the gap widening over time.
The mechanism involves both immediate healing complications and long-term maintenance challenges. Smokers show delayed osseointegration, increased infection rates, and accelerated bone loss around functioning implants. Even light smoking (less than 10 cigarettes daily) significantly impacts outcomes, dispelling the myth that moderate tobacco use is acceptable with implants.
Myth: All implant materials and designs perform identically over time. While quality implants from reputable manufacturers show similar short-term success rates, subtle differences in material properties, surface treatments, and design features affect long-term outcomes. Generic or poorly researched implant systems lack the extensive clinical documentation that supports established brands, creating uncertainty about performance beyond 10-15 years.
Surface characteristics particularly influence longevity. Smooth surfaces, once common in early implant generations, show higher rates of late failure compared to modern textured surfaces. Similarly, implant-abutment connection designs affect bacterial infiltration and mechanical stability over decades of function. Patients receiving well-researched implant systems with documented long-term performance gain significant advantages in predictable outcomes.
Maintaining Long Term Dental Implants for Lasting Success
Successful implant maintenance requires understanding that oral hygiene around implants differs significantly from natural tooth care. While brushing and flossing remain essential, the techniques require modification because implant crowns and supporting structures have different shapes and access requirements than natural teeth. Traditional flossing often proves inadequate around implants, making specialized tools like water flossers, interdental brushes, and implant-specific floss essential for effective cleaning.
Professional maintenance protocols have evolved as practitioners gained experience with long-term implant care. Research indicates that patients following structured maintenance programs—typically involving professional cleanings every 3-4 months rather than the standard 6-month interval—experience significantly better long-term outcomes. These appointments focus on removing bacterial biofilms that home care cannot eliminate and monitoring for early signs of complications.
Lifestyle factors beyond smoking dramatically influence implant longevity. Uncontrolled diabetes impairs healing and increases infection risk, with hemoglobin A1c levels above 7% correlating with higher failure rates. Patients taking certain medications—particularly bisphosphonates for osteoporosis—require modified treatment protocols and enhanced monitoring due to potential healing complications.
Bruxism (teeth grinding) presents a particular challenge for implant longevity because the protective mechanisms present in natural teeth don’t exist around implants. Natural teeth can detect excessive forces and trigger protective reflexes, while implants cannot. This lack of proprioception means grinding forces transfer directly to the implant-bone interface, potentially causing mechanical complications or accelerated bone loss. Night guards and stress management become crucial components of long-term implant success for affected patients.
Managing peri-implantitis when it occurs determines whether implants survive for decades or require removal within years. Early intervention—when gum inflammation appears but bone loss hasn’t progressed—often responds to enhanced hygiene and professional debridement. Advanced cases may require surgical intervention to regenerate lost bone and tissues, though outcomes become less predictable as destruction progresses.
Research Insights and Future Trends in Long Term Dental Implants
Recent longitudinal studies provide unprecedented insight into real-world implant survival rates beyond the controlled conditions of initial clinical trials. A landmark 2024 study following 2,500 implants for 20+ years found that patient compliance with maintenance protocols emerged as the strongest predictor of long-term success—more influential than age, bone quality, or even implant design. This finding reinforces the critical role of patient education and ongoing care in achieving advertised longevity rates.
Surface technology innovations continue advancing implant performance. Current research focuses on bioactive surfaces that not only encourage bone integration but actively promote tissue health over time. Experimental coatings incorporating antimicrobial properties show promise for reducing peri-implantitis risk, while surfaces designed to release beneficial ions may enhance long-term bone maintenance.
Digital treatment planning and computer-guided surgery are revolutionizing implant placement accuracy, directly impacting longevity. Precise three-dimensional positioning optimizes force distribution and tissue architecture around implants, factors that influence decades of function. Early data suggests computer-planned implants show improved long-term outcomes compared to traditional freehand placement, though longer follow-up periods are needed for definitive conclusions.
Emerging regenerative therapies offer potential solutions for patients with compromised bone or soft tissues that previously precluded long-term implant success. Techniques combining implant placement with bone grafting, growth factors, and tissue engineering show promise for expanding implant candidacy while improving long-term stability. However, these advanced procedures require careful patient selection and experienced practitioners to achieve predictable results.
The future of implant longevity increasingly focuses on personalized treatment protocols based on individual risk assessment. Genetic testing for healing capacity, sophisticated imaging of bone quality, and predictive modeling of patient compliance may enable practitioners to customize treatment plans for optimal long-term outcomes. While still in early development, these approaches suggest that implant longevity will continue improving as treatment becomes more individualized and scientifically precise.
Understanding these research trends helps patients and practitioners set realistic expectations while maximizing the probability of decades-long implant success. The data consistently shows that when proper protocols are followed, modern implants can indeed provide reliable function for 20, 30, or even 40+ years—making them a sound investment in long-term oral health and quality of life.